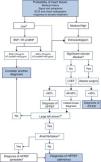
Heart failure (HF) patients present frequently comorbidities and the diagnosis of HF in this setting is a challenge. The symptoms and signs of HF may be atypical and can be simulated or disguised by co-morbidities such as respiratory disease and/or obesity. For this reasons, confirmation of the diagnosis always requires further tests. Natriuretic peptides accurately exclude cardiac dysfunction as a cause of symptoms, but the optimal cut-off levels for ruling out and ruling in HF diagnosis are influenced by different co-morbidities. Echocardiography should be performed in all patients to confirm the diagnosis of HF, except in those cases with low clinical probability and a concentration of brain natriuretic peptides below the exclusion cut-off. This review aims to provide a practical clinical approach for the diagnosis of HF in patients with comorbidity, focusing in older patients and patients with chronic obstructive pulmonary disease and/or obesity.
Los pacientes con insuficiencia cardiaca (IC) con frecuencia presentan comorbilidades que pueden dificultar su diagnóstico. Los signos y síntomas de la IC pueden ser atípicos o difíciles de distinguir de los de otras comorbilidades, como las enfermedades respiratorias o la obesidad. Por ello, para confirmar el diagnóstico suelen ser precisas exploraciones complementarias. Los péptidos natriuréticos permiten excluir de forma adecuada la disfunción cardíaca, pero los puntos de corte óptimos, tanto para la exclusión como para la confirmación diagnóstica de la IC, están influenciados por las distintas comorbilidades. El ecocardiograma deberá realizarse a todos los pacientes para confirmar el diagnóstico de IC, excepto cuando la probabilidad clínica sea muy baja y la concentración de péptidos natriuréticos esté por debajo del punto de corte de exclusión. En esta revisión se proponen recomendaciones prácticas para el diagnóstico de IC en pacientes con comorbilidades, especialmente en el paciente anciano, con enfermedad pulmonar obstructiva crónica u obesidad.
Article
Diríjase desde aquí a la web de la >>>FESEMI<<< e inicie sesión mediante el formulario que se encuentra en la barra superior, pulsando sobre el candado.

Una vez autentificado, en la misma web de FESEMI, en el menú superior, elija la opción deseada.

>>>FESEMI<<<