Evaluation of quality of care for patients with diabetes mellitus admitted to hospitals in Spain.
MethodsCross-sectional study in one day that included 1193 (26.7%) patients with type 2 diabetes or hyperglycaemia out of a total of 4468 patients admitted to the internal medicine departments of 53 hospitals in Spain. We collected demographic data, adequacy of capillary glycaemic monitoring, treatment administered during admission, and recommended therapy at discharge.
ResultsThe median age of the patients was 80 years [74–87], of which 561 (47%) were women, with a Charlson index of 4 points [2–6], and 742 (65%) were fragile. Median blood glucose on admission was 155 mg/dl [119–213]. On the third day, the number of capillary blood glucose levels in target (80−180 mg/dl) at pre-breakfast was 792/1126 (70.3%), pre-lunch 601/1083 (55.4%), pre-dinner 591/1073 (55.0%), and at night 317/529 (59.9%). A total of 35 patients (0.9%) were suffering from hypoglycemia. Treatment during hospitalization was performed with sliding scale insulin in 352 (40.5%) patients, with basal insulin and rapid insulin analogues in 434 (50%), or with diet exclusively in 101 (9.1%). A total of 735 (61.6%) patients had a recent HbA1c value. At discharge, the use of SGLT2i increased significantly (30.1% vs. 21.6%; p < 0.001), as did the use of basal insulin (25.3% vs. 10.1%; p < 0.001).
ConclusionsThere is an excessive use of sliding scale insulin as well as insufficient information on HbA1c values and prescription upon discharge of treatments with cardiovascular benefit.
Evaluación de la calidad de la asistencia a los pacientes con diabetes mellitus ingresados en España.
MétodosEstudio transversal que incluyó a 1193 (26,7%) pacientes con diabetes tipo 2 o hiperglucemia de un total de 4468 pacientes ingresados en los servicios de medicina interna de 53 hospitales (España). Se recogieron datos demográficos, adecuación de la monitorización de la glucemia capilar, tratamiento administrado durante el ingreso y terapia recomendada al alta.
ResultadosLa edad mediana fue 80 años [74–87], 561 (47%) pacientes eran mujeres, con un índice de Charlson de 4 [2–6] puntos, siendo clasificados frágiles 742 (65%). La mediana de glucemia al ingreso fue 155 [119–213] mg/dl. Al tercer día de ingreso el número de glucemias capilares en objetivo (80–180 mg/dl) fue de 792/1126 (70,3%) en el predesayuno, 601/1083 (55,4%) en precomida, 591/1073 (55,0%) en precena y 317/529 (59.9%) durante la noche. Se observó hipoglucemia en 35 (0,9%) pacientes. El tratamiento durante el ingreso fue realizado con insulina en escala móvil en 352 (40,5%) pacientes, insulina basal y análogos de insulina rápida en 434 (50%) y dieta exclusivamente en 101 (9,1%). Un total de 735 (61,6%) pacientes disponían de un valor reciente de HbA1c. En el alta se incrementó el uso de iSGLT2 (30,1% vs. 21,6%; p < 0,001) y el uso de insulina basal (25,3% vs. 10,1%; p < 0,001).
ConclusionesExiste un excesivo uso de insulina en escala móvil, una deficiente información de valores de HbA1c y una prescripción aún deficiente de tratamientos con beneficio cardiovascular al alta.
Diabetes mellitus and hyperglycaemia comprise between 15%–25% of diagnoses in patients admitted to internal medicine departments.1–3 This terminology includes patients with known diabetes mellitus, patients with unknown diabetes, and patients with stress hyperglycaemia, defined as an abnormal elevation of blood glucose that disappears upon resolution of the acute disease.
Data from observational studies and clinical trials show an association between hyperglycaemia and adverse prognosis with regard to mortality, morbidity, hospital stay, infections, and other complications.4–7 There is information indicating that correcting hyperglycaemia reduces the appearance of infections, hospital complications, and mortality.8,9
Antihyperglycemic drugs, such as sulfonylureas, metformin, and thiazolidinediones, are not recommended for hospital use due to the risk of adverse effects.7 Experiences have been reported with other drugs such as dipeptidyl peptidase-4 (DPP-4) inhibitors, sodium-glucose co-transporter-2 inhibitors (SGLT2i), or glucagon-like peptide-1 receptor agonists (GLP-1 RA), but their hospital use is not yet highly widespread.10–12 For in-hospital hyperglycaemia management, the clinical practice guidelines recommend using insulin when glucose levels are greater than or equal to 180 mg/dl (10 mmol/l) confirmed on 2 occasions.7,13 Upon starting treatment, the target is to maintain glucose levels between 140–180 mg/dl (7.8–10 mmol/l), thus preventing hypoglycaemia. During the patient discharge transition, structured scheduling is recommended with a follow-up visit within 30 days or fewer, medication adjustments based on recent HbA1c values, patient education on hypoglycaemia self-monitoring and identification, as well as advice on diet and medication dosing on days of illness. However, adherence to clinical practice guidelines on in-hospital hyperglycaemia treatment and management is not always comprehensive.14
In this domestic study, we analysed the prevalence of diabetes and hyperglycaemia in internal medicine departments, the degree of glucose monitoring, types of drugs used to control blood glucose, incidence of hypoglycaemia, and the suitability of treatment at hospital discharge.
MethodsStudy design and selection criteriaA cross-sectional prevalence study was performed over the course of one day. An email was sent out to members of the Diabetes, Obesity, and Nutrition Workgroup and all members of the Spanish Society for Internal Medicine with an invitation to participate in the study. A plan was made to include patients from a single day selected by the researchers during the periods spanning 24–28 October and 7–11 November 2022. The study involved internal medicine departments from centres included in the 2021 National Catalogue of Spanish Hospitals. Consecutively, we selected patients presenting with diabetes mellitus or hyperglycaemia in the emergency department (blood glucose >180 mg/dl). Patients under the age of 15 and those admitted to critical care units were excluded from the study. The study followed the STROBE reporting recommendations for observational studies.
Data collectionInformation related to the participating hospitals was collected and anonymised, and included location, number of beds, number of admitted patients at the time of the study, and affiliation status with universities.
Patient-related information included age, sex, smoking status, type of diabetes, duration of diabetes since diagnosis, most recent HbA1c value and date, estimated glomerular filtration (CKD-EPI), frailty score, Charlson comorbidity index, diabetes treatment prior to admission, reason for hospitalisation, diabetes treatment administered on the third day of hospitalisation, use of enteral or parenteral nutrition, treatment with systemic glucocorticoids, blood glucose at admission, and capillary blood glucose 72 hours post-admission and presence of hypoglycaemia (blood glucose <70 mg/dl) during hospitalisation.
Analysed outcomesOf the primary outcomes analysed, the follower were evaluated: frequency of blood sugar monitoring adapted to patient intake or medication, insulin use in a basal-bolus protocol or basal-bolus-correction protocol as a hyperglycaemia management method, and recent availability of HbA1c value prior to hospital discharge (in a period of under three months).
As secondary outcomes, the frequency of initial treatment modification based on the presence of cardiovascular disease, heart failure, or kidney disease, was analysed.
Ethical considerationsThe study was conducted in accordance with Spanish legislative requirements regarding biomedical research, data protection, and bioethics. The study was approved by the institutional review board. All the patients gave their informed consent.
Statistical analysisDescriptive statistics were used, calculating the mean and standard deviation for parametric quantitative variables, and median and interquartile range for nonparametric quantitative variables, and absolute number and percentage for qualitative variables. The comparisons between categorical variables were carried out using the chi-squared test. All the analyses were estimated for 2 tails. p Values <0.05 were considered significant.
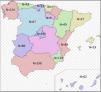
ResultsA total of 53 Spanish hospitals participated in the study, of which 10 (19%) were primary, 20 (38%) secondary, and 23 (43%) were tertiary referral hospitals. All the autonomous communities were represented with the exceptions of Castilla la Mancha and Navarra (Fig. 1). At the time of the study, a total of 4468 adult patients were hospitalised in internal medicine departments in the participating hospitals of which 1193 (26.7%) presented diabetes or hyperglycaemia, classified into type 1 diabetes (N = 14), type 2 diabetes (N = 1053), stress hyperglycaemia (N = 78) or other types of diabetes (N = 48). A total of 156 patients were diagnosed with previously unknown diabetes during admission.
Patient characteristicsThe median patient age was 80 years (interquartile range [IQR]: 74−87), of which 561 (47%) were female (Table 1). The median (IQR) duration of diabetes mellitus from the time of diagnosis was 12 years.6–18 Prior to hospital admission, diabetes treatment was being administered to 606 (51%) patients via oral medication, to 261 (22%) with oral medication and insulin, and to 120 (10%) exclusively with insulin therapy. Regarding oral medication, the most commonly taken were: 557 (47%) metformin, 400 (34%) dipeptidyl peptidase-4 (DPP-4) inhibitors, and 256 (22%) sodium-glucose co-transporter-2 inhibitors (SGLT2i). Only 8 (0.7%) of the patients were receiving treatment with glucagon-like peptide-1 receptor agonists (GLP-1 RA). Regarding reasons for hospital admission, the reason was due to diabetes-related problems in only 50 (4%) patients; for the majority of the patients the reasons for admission were due to infectious disease in 652 (55%), cardiovascular disease in 346 (29%), respiratory disease in 378 (31%), or genitourinary in 231 (19%). The patients presented elevated comorbidity measured by a median (IQR) of the Charlson index of 4 (2–6) points and 742 (65%) presented frailty criteria according to the Frailty scale. A total of 673 (57%) patients presented an estimated glomerular filtration rate of less than 60 mL/min/1.73 m2.
Characteristics of the study population.
| Variable | |
| Age, years | 80 [74−87] |
| Age category | |
| <65 years | 123 (10.3) |
| 65–80 years | 443 (37.1) |
| –>80 years | 627 (52.6) |
| Sex, male | 632 (52.9) |
| Weight, kg | 75 [64−85] |
| BMI | 27.7 [24.3−31.6] |
| Duration of diabetes, years | 12 [6–18] |
| Charlson Index | 4 [2–6] |
| Comorbidities | |
| Heart failure | 501 (41.9) |
| Myocardial infarction | 225 (18.9) |
| Peripheral artery disease | 198 (16.9) |
| Cerebrovascular disease | 310 (26.0) |
| Dementia | 271 (22.7) |
| COPD | 269 (22.5) |
| Connective tissue disease | 65 (5.4) |
| Moderate or severe kidney disease (eFGR < 60 mL/min/1.73 m2) | 412 (34.5) |
| Solid tumour without metastasis | 103 (8.6) |
| Solid tumour with metastasis | 62 (5.2) |
| Moderate-severe liver disease | 44 (3.7) |
| Leukaemia–lymphoma | 28 (2.4) |
| Frailty category | |
| Not frail | 87 (7.6) |
| Pre-frail | 308 (27.0) |
| Frail | 742 (65.2) |
| Treatment prior to admission | |
| Oral medication | 606 (51.3) |
| Oral medication and insulin | 261 (22.1) |
| Insulin | 120 (10.1) |
| Reason for hospital admission | |
| Diabetes-related | |
| Diabetic ketoacidosis | 14 (1.2) |
| Hyperosmolar hyperglycaemic state | 26 (2.2) |
| Hypoglycaemia | 10 (0.8) |
| Not diabetes-related | |
| Infection | 652 (54.9) |
| Respiratory disease | 378 (31.8) |
| Heart disease | 346 (29.1) |
| Genitourinary disease | 231 (19.5) |
| Nervous system disorders | 110 (9.3) |
| Cancer | 104 (8.7) |
| Musculoskeletal disease | 66 (5.6) |
| Others | 206 (17.6) |
The values are expressed as median (interquartile range) or frequency (percentage).
At the time of admission, the median blood sugar value in the emergency department was 155 mg/dl [119–213.5], with 62% of the values below 180 mg/dl (Table 2). During hospitalisation, blood glucose monitoring was performed at bedside with portable blood glucose meters. Over the course of the third day of admission, a total of 3811 capillary blood glucose measurements were taken, corresponding to an average of 3.2 measurements per patient and day. The number and frequency of capillary blood glucose measurements performed before breakfast was 1126 (94%), before the midday meal or lunch 1083 (91%), before dinner 1073 (90%), and at night 529 (44%). The number of blood glucose readings in the optimal range (80−180 mg/dl) obtained before breakfast, lunch, dinner, and at night were 70.3%, 55.4%, 55.0% and 59.9%, respectively (Fig. 2). On the third day of hospital admission, hypoglycaemia (blood glucose <70 mg/dl) was observed in 35 (0.9%) patients. No values considered to be severe hypoglycaemia (blood glucose <54 mg/dl) were detected during admission. A total of 98 (8.2%) patients died during hospital admission.
Blood glucose monitoring and treatment administered during hospital admission.
| Blood glucose in emergency department, mg/dl | 155 [119−213] |
| Blood glucose category in the emergency department | |
| <180 mg/dl | 740 (62.3) |
| ≥180 mg/dl | 448 (37.7) |
| Number of capillary blood glucose measurements on day 3 of admission | |
| Before breakfast | 1126 (94.3) |
| Before lunch | 1083 (90.8) |
| Before dinner | 1073 (89.9) |
| Night | 529 (44.3) |
| Capillary blood glucose at day 3 of admission, mg/dl | |
| Before breakfast | 140 [110−181] |
| Before lunch | 168 [130−225] |
| Before dinner | 170 [133−225] |
| Night | 160 [124−205] |
| Hypoglycaemia (Glucose <70 mg/dl) | 85 (2.2) |
| Insulin dose, units/day | |
| Basal insulin | 12 [10–20] |
| Prandial or correction insulin | 8 [4–14] |
| Recent HbA1c value, % | |
| <6.5 | 306 (41.6) |
| 6.5−7.0 | 135 (18.3) |
| 7.1−8.0 | 155 (21.1) |
| 8.1−9.0 | 82 (11.2) |
| >9.0 | 57 (7.8) |
The values are expressed as median (interquartile range) or frequency (percentage).
Blood glucose was managed during hospitalisation with oral antihyperglycemic agents in 26 (2%) patients, oral antihyperglycemic agents and insulin in 172 (15%) patients, and insulin in 870 (74%) patients. A total of 25 (2%) patients did not receive hyperglycaemia treatment while in hospital. In terms of insulin administration, 434 (50%) patients were treated with basal insulin and prandial insulin correction doses, 352 (40%) patients were treated with sliding scale insulin, and 82 (9%) patients with basal insulin. The median dose of basal insulin was 12 U10–20 per day and that of prandial insulin was 8 U4–14 per day. A total of 735 (61%) of the patients had a recent HbA1c value, of which 306 (42%) patients had HbA1c values below 6.5%, while 57 (8%) had HbA1c values above 9%.
Treatment modifications at hospital dischargeAt discharge, treatment modifications were made compared to the treatment protocols which the patients had at the time of admission (Table 3). We observed a significant reduction in the prescription of sulfonylureas and a significant increase in the prescription of SGLT2i and insulin. We did not observe any significant changes in the prescription of metformin, repaglinide, pioglitazone, or GLP-1 RA.
Medications used prior to hospital admission and changes made at hospital discharge.
| Drug | Prior to admission | At discharge | p |
|---|---|---|---|
| Metformin, no (%) | 557/1186 (46.9) | 472/1045 (45.1) | 0.395 |
| Sulfonylurea, no (%) | 53/1183 (4.48) | 26/1040 (2.50) | 0.011 |
| Repaglinide, no (%) | 77/1184 (6.5) | 49/1045 (4.6) | 0.064 |
| Pioglitazone, no (%) | 9/1182 (0.7) | 8/1039 (0.7) | 0.981 |
| iSGLT2, no (%) | 256/1184 (21.6) | 315/1045 (30.1) | <0.001 |
| AR-GLP1, no (%) | 58/1181 (4.9) | 59/1009 (5.6) | 0.331 |
| Only oral medication, no (%) | 606/1181 (51.3) | 519/1044 (49.7) | 0.451 |
| Oral medication and insulin, no (%) | 262/1181 (22.1) | 124/1044 (11.8) | <0.001 |
| Insulin only, no (%) | 120/1181 (10.1) | 265/1044 (25.3) | <0.001 |
This study was carried out in order to identify areas for improvement in care for patients with diabetes mellitus or hyperglycaemia who are hospitalised in internal medicine departments. In terms of patient characteristics what could potentially affect achieving blood glucose targets, notable aspects were a median age of 80, hight rate of cardiovascular and kidney disease, and frailty among 65% of the population. The third day of admission was chosen for measuring the frequency of capillary blood glucose monitoring, the degree of blood glucose control, and antihyperglycemic treatment administered during admission. The study data showed that the number of capillary blood glucose measurements was adapted to nutritional requirements in most of the patients, blood glucose targets were achieved in 70% of the measurements before breakfast and in 55%–60% at the other times of day. Blood glucose was managed in 50% with a basal insulin and prandial insulin protocol, although 40% of patients were treated exclusively with sliding scale insulin. A total of 62% of patients had a recent glycated haemoglobin value to enable treatment adjustments compared to the established blood glucose targets. At discharge, SGLT2i drug prescribing increased by 10% and insulin use by 15%.
Compared to a similar study conducted in 2015 in Spain that included 1000 hospitalised patients with diabetes mellitus or hyperglycaemia, the patients in our study were older in age and had a higher degree of disability.14 The current study stands out for the scarce use of SGLT2i and GLP- 1 RA drugs in a high cardiovascular risk population, as recommended by the guidelines.15,16 Various studies have confirmed the existence of a delay between the publishing recommendations of clinical practice guidelines, supported by strong evidence, and their incorporation into regular clinical practice.17–19 However, hospital admission should represent an opportunity to optimise treatment at the time of discharge. While the use of SGLT2i increased by 10% in our study, its indication for use can be extended to a larger population, analogous to the almost anecdotal use of GLP-1 RAs.
The determining factors for achieving optimal blood glucose management during admission are the blood glucose values observed upon admission to the emergency department and on the third day of hospitalisation, preventing the onset of hypoglycaemia.20 In our study, 62.2% of patients presented blood glucose values below 180 mg/dl in the emergency lab tests. The use of metformin, DPP-4 inhibitors, and SGLT2i during hospitalisation was 2.9%, 7.2% and 7.6%, respectively. Metformin is a drug whose use is often continued in hospitalised patients. However, it should be suspended upon hospital admission due to the risk of lactic acidosis, particularly in patients with sepsis, shock, or kidney or liver failure.21
For patients with mild hyperglycaemia (<200 mg/dl), the use of rapid insulin analogues every 6 hours can be sufficient for blood glucose control, provided they are patients with type 2 diabetes since patients with type 1 diabetes should continue with an intensive basal-bolus insulin protocol.22,23 For patients who have not received insulin prior to hospital admission, the use of DPP-4 inhibitors with corrective doses of rapid insulin every 6 hours or with meals is suggested, as it manages levels in a similar manner to basal-bolus therapy and with less risk of hypoglycaemia.21,24 Regarding SGLT2i use, it is highly likely that these could be incorporated into hospital treatment to not only manage blood sugar, but also to treat heart failure, given the efficacy demonstrated in multiple clinical trials.25,26 The use of other non-insulin injectable therapies for inpatient blood sugar management is being evaluated, including GLP-1 RA, although there is little available evidence to date to recommend it.27 For patients with moderate hyperglycaemia (blood glucose 201–300 mg/dl), insulin therapy at a dose of 0.2–0.3 units per kg/day is recommended, provided the patient is not frail, elderly, or in renal failure, in which case the initial insulin dose should be 0.15 units per kg/day.21 In admitted patients with severe hyperglycaemia (blood glucose >300 mg/dl), the suggested treatment is 0.3 units of insulin per kg/day or to reduce by 20% the total insulin dose received by the patient.
The capillary blood glucose results obtained on the third day of admission indicate a margin of improvement, with 70% of pre-breakfast values within the therapeutic target range, though this was only achieved in 55%–60% of the remaining measurements throughout the day. These data indicate an appropriate choice of basal insulin dose and poor management of prandial blood glucose, potentially due to caution in preventing hypoglycaemia. The daily doses of basal and prandial or correction dose insulin administered presented a median value of between 12 and 8 units per day, respectively. This insulin dose (median value 0.27 units per kg/day) indicates significant therapeutic caution to prevent potential hypoglycaemia in an older population with severe comorbidities and an elevated degree of frailty. For these patients, the clinical practice guidelines advise avoiding hyperglycaemia symptoms and the onset of hypoglycaemia.28 For frail patients or patients in nursing homes, glucose control targets are random blood glucose values between 100 and 200 mg/dl.29 The prevalence of hypoglycaemia on the third day of hospital admission was 2%. This hypoglycaemia figure was similar to that reported in other studies using continuous glucose monitoring.29
In summary, with this descriptive study we were able to identify areas for improvement in inpatient care in internal medicine departments. The use of oral therapies for blood sugar control during hospitalisation is still lacking and could contribute to reducing insulin doses and the risk of hypoglycaemia. On the other hand, we identified that a significant number of patients do not have a recent HbA1c value, which limits opportunities to achieve therapeutic targets. Lastly, hospitalisation is not taken as an opportunity to adjust diabetes treatment at discharge according to the clinical practice guideline recommendations. However, it must be noted that the obtained results are biased in that they were collected by a group of researchers with a specific interest in diabetes and blood sugar management.
FundingLaboratorios Novo-Nordisk provided the funds to develop the electronic data collection form. Novo-Nordisk has no relation to the study design nor the data collection, analysis, or interpretation, nor the writing of the manuscript or decision to send it for publication.
Conflicts of interestEthical aspects: the study protocol was approved by the Badajoz University Hospital Research Committee. The obtained information was deidentified according to the recommendations of the Data Protection Law. The patients signed the informed consent.